Frozen Shoulder and Menopause: Why Your Shoulder Might Feel Locked – and How to Get It Moving Again
Hello, lovely. If you’re in your forties or fifties and you’ve suddenly noticed one shoulder feeling tight, achy and strangely reluctant to lift or rotate, you’re probably wondering what on earth is going on. You haven’t had a big injury. You’re not training for a marathon. Yet reaching for your bra strap or brushing your hair has become a wince-worthy challenge. Sound familiar?
You’re not imagining it, and you’re far from alone. Frozen shoulder and menopause often arrive hand-in-hand, and the connection is stronger than many realise. In this in-depth, 2500-word guide I’ve pulled together the latest science (including 2022–2025 studies from Duke Health and the North American Menopause Society), real-women stories, practical exercises and gentle lifestyle changes that actually help. No jargon, no fluff – just honest, hopeful information in simple British English so you can start feeling better today.
Let’s thaw this together.
What Exactly Is Frozen Shoulder (Adhesive Capsulitis)?
Frozen shoulder, or adhesive capsulitis, happens when the capsule of connective tissue surrounding your shoulder joint becomes thick, inflamed and tight. The normally loose, stretchy “bag” that lets your arm swing freely shrinks and sticks, literally freezing the joint.
It usually affects only one shoulder, though the other can follow months later. Women between 40 and 60 are hit hardest – up to four times more often than men – and the peak age sits right in the middle of perimenopause and early menopause.
Normal shoulder vs frozen shoulder – you can see how the inflamed capsule (shown in red) restricts movement.
The Menopause Connection: It’s Not “Just Ageing”
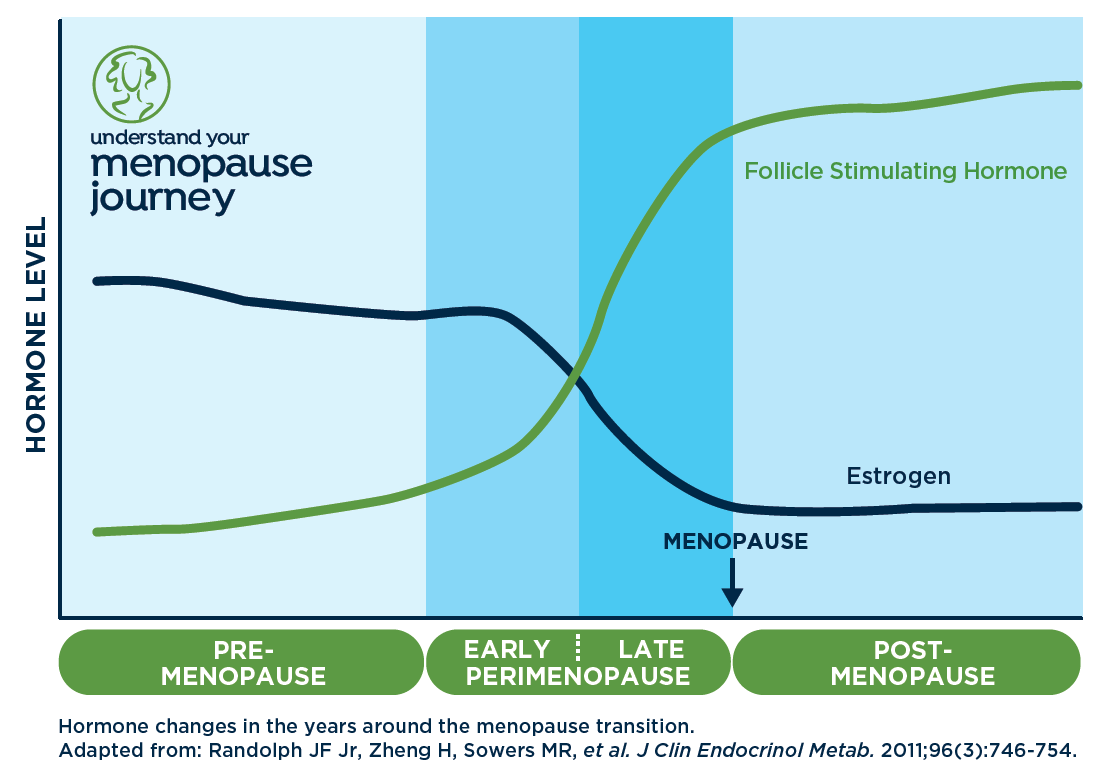
During perimenopause and menopause, oestrogen levels drop dramatically. Oestrogen isn’t only about periods and hot flushes – it plays a starring role in keeping your connective tissues supple, your collagen production healthy and inflammation in check.
When oestrogen declines, the shoulder capsule can become more prone to inflammation and scarring. Research presented at the North American Menopause Society in 2022 and later studies (including a 2025 Duke Health analysis) found that women not taking systemic hormone therapy had nearly double the odds of developing frozen shoulder compared with those who were.
One 2022 Duke retrospective study of almost 2,000 postmenopausal women showed only 3.95 % of those on hormone therapy developed adhesive capsulitis versus 7.65 % of those who weren’t. While larger trials are still needed, the pattern is clear: the hormonal shift of menopause is a significant risk factor for frozen shoulder.
Check here your useful resource
Other menopause-related changes pile on too – reduced muscle strength around the shoulder, poorer sleep (which heightens pain perception), and the natural tendency to move less when joints ache, which unfortunately makes stiffness worse.
The beautiful hormone chart above shows exactly when oestrogen takes its steepest dive – right when frozen shoulder risk climbs. Check here your useful resource
Recognizing the Symptoms of Frozen Shoulder in Menopause
The condition unfolds in three distinct stages:
- Freezing (Painful) stage – lasts 2–9 months. Sharp pain at night, even at rest. Reaching overhead or behind your back hurts most. Many women describe it as “someone tightening a screw inside my shoulder”.
- Frozen (Stiff) stage – 4–12 months. Pain eases a little but stiffness peaks. You can barely lift your arm or put on a coat without help. Check here your useful resource
- Thawing (Recovery) stage – 5–24 months (or longer). Gradual return of movement. Full recovery can take 1–3 years, but most women regain 80–90 % function with the right care.
Common daily frustrations during frozen shoulder and menopause:
- Can’t fasten your necklace
- Struggle to wash your hair
- Pain when rolling over in bed
- Difficulty driving or reaching the seatbelt
If any of these ring bells, don’t wait – early intervention shortens the whole miserable journey.
Who Is Most at Risk?
- Women 40–60 in perimenopause or post-menopause
- Those with diabetes (risk jumps to 10–20 %)
- Thyroid disorders
- Previous shoulder injury or surgery
- Prolonged immobility (e.g., after illness or fracture)
- Asian ethnicity (higher reported rates)
How Doctors Diagnose It
Your GP or physiotherapist can usually diagnose frozen shoulder from your story and a simple physical exam (they’ll check external rotation – the movement most restricted). X-rays rule out arthritis; ultrasound or MRI are sometimes used if the picture isn’t clear.
Treatment Options That Actually Work
1. Pain Relief & Anti-Inflammatories
Paracetamol, ibuprofen (if safe for you) and topical gels. Short courses of oral steroids in the freezing stage can calm the fire quickly.
2. Physiotherapy – But Timing Matters
Aggressive stretching in the freezing stage can worsen inflammation. Gentle pendulum swings and passive movements are better early on. Once in the frozen stage, more intensive stretching and strengthening begin.
3. Injections
Corticosteroid injection into the joint or hydrodilatation (injecting saline to stretch the capsule) can dramatically speed recovery when done at the right moment.
4. Hormone Therapy Discussion
The emerging evidence that systemic oestrogen may halve risk or ease symptoms means it’s worth a conversation with your GP or menopause specialist – especially if you have other menopause symptoms. Always weigh personal risks and benefits.
5. Advanced Options (Rarely Needed)
Manipulation under anaesthetic or arthroscopic release for stubborn cases.
Most women recover well with conservative care plus patience.
Gentle Exercises to Start Today (Safe for Menopause)
Do these daily, slowly, and stop if pain sharply increases. Breathe deeply – tension makes everything worse.
Aim for consistency over intensity. Many women notice improvement within 4–6 weeks of daily gentle work.
Lifestyle Changes That Support Shoulder (and Whole-Body) Health in Menopause
- Stay gently active – walking, swimming, yoga. Movement prevents the next joint from freezing.
- Anti-inflammatory eating – oily fish, berries, turmeric, leafy greens, olive oil. Cut ultra-processed foods and excess sugar (especially important if you have diabetes risk).
- Strength train – light weights or resistance bands twice weekly for upper back and shoulders.
- Sleep well – magnesium glycinate or tart cherry can help; poor sleep amplifies pain.
- Manage stress – chronic cortisol worsens inflammation. Even 10 minutes of breathing or mindfulness daily helps.
- Maintain healthy weight – extra kilos increase load on joints.
- Check here your useful resource
Group walks or outdoor movement with friends – pure medicine for both body and soul.
Frequently Asked Questions About Frozen Shoulder and Menopause
Final Thoughts: You’ve Got This
Frozen shoulder during menopause can feel like one more unfair blow when you’re already navigating hot flushes, sleep disruption and mood swings. But here’s the hopeful truth: this phase passes. With the right knowledge, gentle movement, timely medical support and self-compassion, most women regain full or near-full use of their shoulder and come out stronger, more in tune with their changing bodies.
You are not “falling apart”. Your body is going through a profound transition, and it’s asking for kindness, movement and understanding – not punishment or ignoring the signals.
If you’re struggling right now, start with one small thing today: a five-minute pendulum swing while the kettle boils, a walk with a friend, or booking that GP appointment you’ve been putting off. You deserve to move freely again – reaching for the stars (or at least the top shelf) without wincing.
You’ve already taken the first step by reading this far. Keep going. The thaw is coming.











Comments
Post a Comment